Mould Illness: A UK Functional Medicine Approach 2023

This article summarises mould illness and provides strategies for healing from it, with links to UK-based (and many US) testing and cleaning companies. It forms a ‘master blog’ on mould illness and includes links to many other blogs I have written on specific elements of testing and treatment. You can check out all my blogs on mycotoxins here, and you may be particularly interested in:
- 5 Things To Know When Living In Mould.
- Mycotoxin Testing: Everything You Need To Know
- Can Mould And Mycotoxins Cause Chronic Fatigue Syndrome?
- Detoxify Mould And Mycotoxins With Lipomsomal Glutathione
If you are a practitioner who would like to become mould literate then I highly recommend Dr. Jill Crista’s professional training. Get 10% off with code alexmanos.
What Is Mould Illness?
Put simply mould illness is when someone is exposed to toxic mould and develops symptoms. It is sometimes referred to a ‘sick building syndrome’ and can lead to a conditions called chronic inflammatory response syndrome. One of the ways mould exposure can cause illness is through their production of mycotoxins. Mycotoxins are metabolites of mould that we breath in.
The world health organisation defines mycotoxins as “naturally occurring toxins produced by certain moulds (fungi) and can be found in food.”
Yes, we are exposed to mycotoxins through our food. But perhaps more preoblematic to our health is when we are exposed to a water damaged property (because of a leak or damp issue) resulting in us breathing in large quantities of these toxins.
For a more in depth article read The Ultimate Guide to Mycotoxins and for more specific information on specific mycotoxins check out these blogs:
Types Of Mould And Mycotoxins
There are three main genera usually tested: Aspergillus, Fusarium, Stachybotrys – there are hundreds of known mycotoxins within these genera.
- Aspergillus is the most prevalent mold group in the environment. Two of the most common Aspergillus mycotoxins are aflatoxin and ochratoxin. The main target of these toxins is the liver.
- Fusarium’s major mycotoxins are zearalenone (ZEN) and fumonisin. Exposure to mycotoxins from Fusarium can lead to both acute and chronic effects.
- Stachybotrys is a greenish-black mold. Two of the more frequently produced by Stachybotrys are roridin E and verrucarin.
What Are The Symptoms Of Mould Illness And Mycotoxins?
The symptoms of mould illness are extensive.
Mycotoxins are neurotoxic, immune toxic, gut toxic, skin toxic, liver and kidney toxic, and gene toxic.
So symptoms can range from insomnia to irritable bowel syndrome (and thus chronic SIBO), chronic fatigue, liver dysfunction, and leaky gut, skin conditions such as rashes, red eyes, coughing, headaches, and autoimmune diseases.
Dr. Crista has an online quiz to help you establish the likelihood of suffering with mould illness: click here.
How Do You Test For Mould And Mycotoxins In The UK?
To look specifically at mycotoxins there is a urinary mycotoxin test available. Currently two labs offer this test – one is Mosaic Diagnostics, the other is Real Time Labs. They have their own pro’s and con’s. You can learn more about testing mycotoxins by reading my blog “Testing Mycotoxins: Everything You Need To Know“.
In a great paper by Dr. Pizzorno he explains how genetic testing may help to identify those most susceptible to mold toxins and other environmental toxins. I’m a big fan of Lifecode GX who offer genetic testing (via working with a practitioner). Running the Lifecode GX test helps us understand our genetic predispositions that might influence our capacity to detoxify mycotoxins. This can then help tailor treatment to the individual.
It is also recommended to assess for potential nutritional deficiencies and levels of other environmental toxins that may help identify those with increased individual susceptibility. In fact the research says that the determining factor as to whether someone will get ill from mould is the exposure itself (how much and how long) and their health status at the time of the exposure.
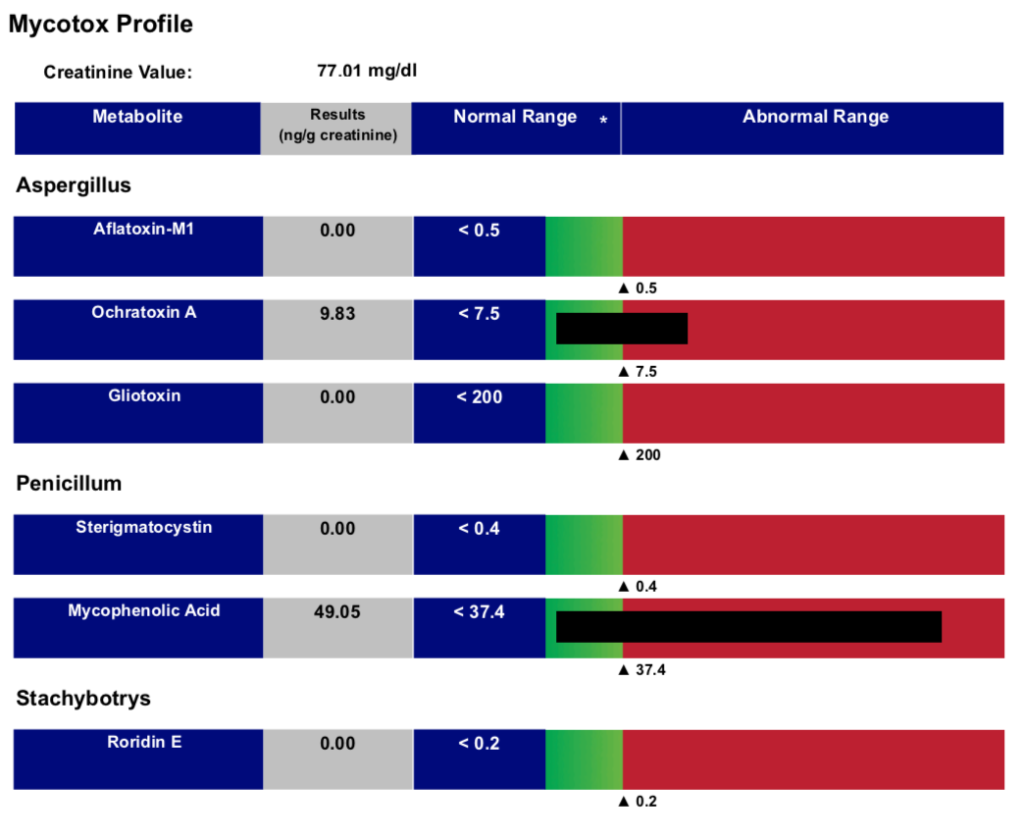
A sample of a urine mycotoxin profile can be found below:
Understanding Mycotoxin Testing
Watch the below video or/and read my blog post Mycotoxin Testing: Everything You Need To Know to learn about the mycotoxin test.
Common Sources of Mould Exposure In The Home
According to Great Plains Laboratory, a US based lab which offer the above mycotoxin test, common exposures may include:
- Window sills and doors
- Plumbing
- Bathrooms
- Closets
- Fireplaces and chimneys
- Laundry rooms
- Basements
- Air conditioning systems
- Roofs
- Refrigerators
Home Inspection And Treatment
Improving air quality is important. I recommend investing in an air purifier and dehumidifier for this purpose.
The dehumidifer I recommend can be found on Amazon, click here.
You may also like to check out Action Dry who, as discussed in my blog, I have used personally when we had a mould issue in our home.
Conscious spaces have some brilliant products including a spray, a detergent and cleaning wipes. All powered by their lab-tested and proven blend of citrus seed extracts.
How Do You Treat Mould Illness?
There are numerous layers to treatment – it really does need to be tailored to the individual based on their unique health state. I will highlight a few common interventions in this article.
You will likely read on various blogs and hear on various podcasts that:
The first step is you must remove yourself from the environment if you are currently being exposed to mould/mycotoxins.
There is a saying in Functional Medicine which is: “you can’t get well in the environment that made you sick”. Nowhere is this more true than with mould illness.
HOWEVER – this is just not realistic for A LOT of people.
And whether you need to move, and how much remediation needs to be done, depends on the magnitude of the problem. I have seen countless clients improve their health (some a little, some a lot) without having to move or remediate. Context, obviously, matters. This should be obvious but I have spoken to people who decided to do nothing when in fact there are things you SHOULD do if you are stuck living in mould.
Learn From Dr. Jill Crista
Watch my interview with leading expert Dr. Jill Crista.
Diet: What Foods Contain Mycotoxins?
There are room foodstuffs that are known to be frequently contaminated with mould and mycotoxins and these include:
- Coffee unless it is tested. I recommend Exhale Coffee as it is tested to be sure it is free from mould, mycotoxins, heavy metals and pesticides.
- Dried fruit.
- Certain grains – wheat, corn, oats, rye.
- Nuts – tree nuts, peanuts, pistachios, Brazil nuts
- Sunflower seeds.
- Certain spices.
- Alcohol – wine, beer.
- Potatoes.
- Milk, cheese and eggs.
It can also be important to avoid foods that might exacerbate imbalances in the gut microbiome (very common when suffering with mould illness). These include:
- Alcohol.
- Sugary foods and drinks
- Mushrooms (although there isn’t a consensus on whether these need to be avoided).
It’s important to appreciate that, in theory, governments have policies in place to ensure our food is safe and we are being exposed to very low levels (you could say acceptable amounts) of mycotoxins. We do see though that studies from various countries around the world (including Europe) have found mycotoxins detected in various bodily fluids of the population. Yet another reason to focus on eating local and in senses produce.
We can also use certain foods, such as ground flaxseed, to bind toxins. Use code ALEXMANOS10 to receive £10 off your orders at Welleasy.
Supplement Considerations
My UK audience can get 10% off your supplements at Healthpath using code ‘alexmanos10’.
My U.S audience might liek to check out Dr. Jill crista’s very own custom formulations.
It’s important to appreciate that there are specific products for specific mycotoxins and therefore a treatment plan needs to be tailored to your individual needs, and the mycotoxins that have come back positive in your mycotoxins test. The below are broad considerations that may be helpful for many, but certainly not all. You may like to refer to my blog on the specific mycotoxin that you are needing to treat.
Liposomal Glutathione
Evidence for the role of oxidative stress in the pathophysiology of mycotoxin-related illness is increasing. The glutathione antioxidant and detoxification systems play a major role in the antioxidant function of cells. Exposure to mycotoxins in humans requires the production of glutathione on an “as needed” basis. Research suggests that mycotoxins can decrease the formation of glutathione due to decreased gene expression of the enzymes needed to form glutathione. Mycotoxin-related compromise of glutathione production can result in an excess of oxidative stress that leads to tissue damage and systemic illness. (source)
- Recommend Product (U.K): Glutathione
- Recommended Product: (U.S.A) Glutathione
Anti-Fungals
It’s very possible that an individual will become colonised with mould, resulting them becoming their very own ‘mobile mouldy property’. This is why it’s possible to still be ill years after moving property.
Options to consider, depend on the mycotoxin present but might include oregano oil or neem.
- Recommend Product (U.K): Biocidin
- Recommended Product: (U.S.A): Oregano oil – I prefer to use multi=herb formulas but don’t have access to any of my preferred options for those in the US. Pau’darco, monolaurin, garlic are other appropriate options though.
Sinus Treatment
The sinuses are the most common site to be colonised with mould. And so sinus treatment is essential for many.
Bitters
Bitters support detoxification and digestion. They do this by supporting bile. What’s interesting is that bile has anti-bacterial properties and thus protective against conditions such as small intestine bacterial overgrowth. SIBO is very common in people with mould illness.
Phosphatidylcholine
Dr. Crista says if there was one edit she could make to her book Break The Mold it would be to add phosphatidylcholine to her recommendations. It aids the detox of mycotoxins as it helps stimulate and thin bile. It also supports cellular health.
- Recommend Product (U.K): Phosphatidylcholine
- Recommended Product (U.S.A): Phosphatidylcholine
Sequestering Agent (Binders)
Sequestering agents refer to non-absorbable materials capable of binding toxins in the gastrointestinal tract, thus reducing the body burden of toxins. These agents are not absorbed into systemic circulation; therefore, side effects are typically limited to gastrointestinal symptoms and potential malabsorption of medications and nutrients, especially if the dose is poorly timed.
Several agents have shown specific efficacy in lowering mycotoxin and endotoxin levels including cholestyramine (a medication), activated carbons (charcoal), and chlorella. Additionally, these agents are nonspecific and can bind additional toxins, helping to lower ‘total body burden’ of toxins.
Probiotics
The ability of Lactobacillus plantarum and Lactobacillus rhamnosus GAF01 to degrade or bind aflatoxin M1. Lactobacillus rhamnosus GG and Lactobacillus casei have a significant hepatoprotective effect against aflatoxin B1. Mycotoxins have also been shown to disrupt the integrity of the gut lining (i.e cause leaky gut) – another reason why probiotics might be helpful.
- Recommend Product (U.K): Probiospore
- Recommended Product: (U.S.A) Probiotics
Omega 3 Fats
Omega 3 fats are helpful at ‘diluting’ the toxins which build up in the fatty parts of our mitochondria, cells, organs and body. This tip came from my conversation with Dr. Jill Crista, a specialist in mycotoxins.
- Recommend Product (U.K): Omega 3 fats
- Recommended Product: (U.S.A) Omega 3
Additional Options
Anti-inflammatories and anti-oxidant compounds such as zinc, NAC, resveratrol, and alpha-lipoic acid.
Sweating: Sauna therapy, hot baths or/and exercise are all appropriate for this. Human sweat has found to contain mycotoxins!
Vivien’s Recovery Story
What To Do When You Can’t Tolerate Supplements
Sometimes people become incredible sensitive to their environment, including food and supplementation. In this situation I find The Gupta Program a really helpful step back to good health.
There are three randomised control trials (so the best level of evidence) evidencing the efficacy of the approach in chronic fatigue syndrome, long COVID, and fibromyalgia.
I have interviewed the founder and CEO Ashok Gupta:
Resources When Suffering With Mould Illness
A great book on mycotoxins and mould illness is Break The Mood by Dr. Jill Crista. Click here.
References For Mould Illness
- Mycotoxin: Its Impact on Gut Health and Microbiota: click here.
- Occurrence and Human-Health Impacts of Mycotoxins in Somalia: click here.
- Biomonitoring in Human Breast Milk: click here.
- Detection of mycotoxins in patients with chronic fatigue syndrome: click here.
- Is Mold Toxicity Really a Problem for Our Patients? Part 2—Nonrespiratory Conditions: click here.
Alex is a certified Functional Medicine Practitioner (IFMCP) and has a MSc in Personalised Nutrition. He is also a breathwork facilitator with a background in personal training and massage therapy. He also runs The Resiliency Program - a 24 week program aimed at building physical, mental, emotional, and spiritual resilience.