I know through personal experience that ‘what happens in the gut doesn’t stay in the gut”. This blog post both shares my own personal experiences of a gut-brain and gut-body connection, but also some of the research answering the question ‘can gut health affect mental health?’, and if probiotics might be helpful for some.
Other blogs that you might be interested in include:
- Nootropics
- Microdosing psychedelics
- Depression: A Functional Medicine Approach
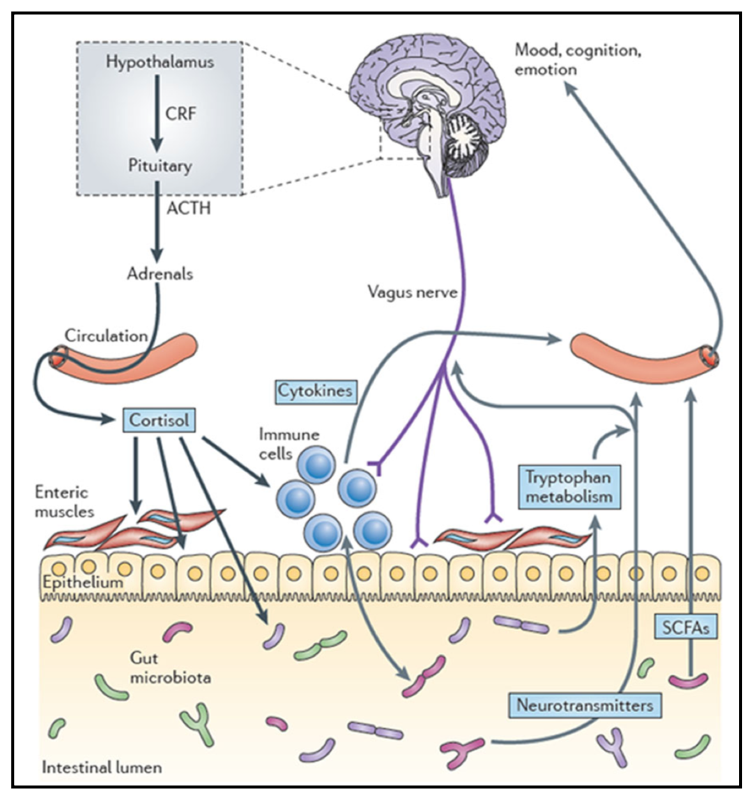
- What Is The Gut-Brain Axis
Can Gut Health Affect Mental Health?
I’ve suffered with psoriasis, acne, terrible dandruff, brain fog, fatigue and for a very short period anxiety. While the gut might not have been the only thing contributing to these conditions, I am 100% confident they were a big part, especially in the anxiety. Let me share a quick story.
About three years ago I was driving home with my, at the time, girlfriend to see my family. Life was good. It was a sunny day, I was looking forward to seeing my family and we were in our Mazda MX5, roof down, and great music pumping through the speakers. We loved that car and have some great memories with it. However, I had this deep anxiety that started in my gut, and slowly rose to my chest. I had no reason to feel anxious, but nonetheless I was. To be honest, I brushed it off and eventually it dissipated.
Then a few days later I was on the train traveling up to clinic and I experienced even worse anxiety – I nearly got off at a random stop because I was feelings anxious. I managed to breath myself out of it though. But it was severe enough for me to know something wasn’t right. I was having some low level gut symptoms at the time – a little bloating and irregular bowel movements so I decided to run a stool test.
The results showed very high levels of the bacteria klebsiella pneumonia. This is a gram-negative bacteria which contains something on its surface called LPS which, under the right circumstances, is pro-inflammatory. Inflammation can contribute to anxiety.
I went through a relatively basic program of supplementing probiotics, prebiotics, and using a broad spectrum anti-microbial that included herbs such as oregano oil, and I haven’t experienced anxiety since. I am convinced this organism, within the context of my health and life at the time, was contributing to some low-level chronic, systemic inflammation that was influencing my mood.
Now I’ll be the first to admit that I don’t think it’s common that one organism drives dis-ease. The relationship between the host (in this case me) and the organism matters most. So variables such as nutrient status, stress levels, the integrity of the gut lining (aka leaky gut), sleep all matter. But in this case I feel like most areas were good, not perfect but not something I needed to particularly change.
So, putting that bit of anecdotal evidence aside, what does the research show us about this connection?
A study published in the reputable medical journal Nature Microbiology provides some of the strongest evidence yet to show that a person’s gut health and microbiome can influence their mental health. The authors used DNA sequencing to analyse microbiota in the faeces of more than 1,000 people enrolled in Belgium’s Flemish Gut Flora Project. The team then correlated different bugs with the participants’ quality of life and incidence of depression, using self-reported and physician-supplied diagnoses.
The researchers found that two groups of bacteria, Coprococcus and Dialister, were reduced in people with depression. And they saw a positive correlation between quality of life and the potential ability of the gut microbiome to synthesise a breakdown product of the neurotransmitter dopamine, called 3,4-dihydroxyphenylacetic acid.
Butyrate-producing Faecalibacterium and Coprococcus bacteria were consistently associated with higher quality of life indicators.
A systematic review of gut microbiota and major depression published in 2019 concluded:
“No consensus has emerged from existing human studies of depression and gut microbiome concerning which bacterial taxa are most relevant to depression. This may in part be due to differences in study design. Given that bacterial functions are conserved across taxonomic groups, we propose that studying microbial functioning may be more productive than a purely taxonomic approach to understanding the gut microbiome in depression.”
The challenge with research is that we are starting to understand the complexity and bioindividuality of humans. Could it be that there isn’t a standard microbiome that contributes to depression – imbalances in one persons microbiome are going to be different in another and thus perhaps we aren’t asking the right question?
Probiotics For Depression
Another layer of evidence demonstrating that our gut health and microbiome can affect our mental health comes from looking at the role of probiotics.
The conclusion of one paper is that “the evidence for probiotics alleviating depressive symptoms is compelling but additional double-blind randomized control trials in clinical populations are warranted to further assess efficacy“.
A systematic review concluded that: “probiotics were associated with a significant reduction in depression”
However not all research is positive. One meta-analyses concluded: “Probiotic supplementation has an overall insignificant effect on mood. Future studies should be conducted on more patients with clinically diagnosed depression”
I have personally found supplementing probiotics and probiotics seem to influence by mood. I am not sure I can succinctly describe the changes but they are there nonetheless. An overall improvement in wellbeing ultimately.
If you want to consider supplementing probiotics then options include:
- Ideal Bowel Support by Jarrow
- BioMe Barrier by Invivo
How Do Probiotics Work In Depression?
In terms of neurotransmission, several rodent studies found that consumption of probiotics prevented stress-induced increases in the hormone adrenocorticotropic hormone (ACTH), corticosterone, adrenaline, and noradrenaline.
The reduction in these markers of chronic stress suggests that treatment with probiotics attenuated the HPA axis, which is hyperactive in depressed patients. Consumption of probiotics was also shown to increase expression of brain-derived neurotrophic factor (BDNF), a growth factor crucial for brain plasticity, memory, and neuronal health that is abnormally reduced in patients suffering from depression.
Other preclinical studies have noted changes in the molecules involved in the biosynthesis and metabolism of the critical neurotransmitter serotonin.
Probiotics have also been shown to possess both antioxidant and free radical scavenging abilities, increase production of GABA, and improve absorption of other nutrients, all of which have been implicated in the pathophysiology of depression.
Research has also discussed probiotics modulating the inflammatory response. The available evidence suggests that “probiotics should be considered a promising adjuvant treatment to reduce the inflammatory activation commonly found in MDD.” Inflammation is a known contributory factor to depression.
Resources
Alex is a certified Functional Medicine Practitioner (IFMCP) and has a MSc in Personalised Nutrition. He is also a breathwork facilitator with a background in personal training and massage therapy. He also runs The Resiliency Program - a 24 week program aimed at building physical, mental, emotional, and spiritual resilience.